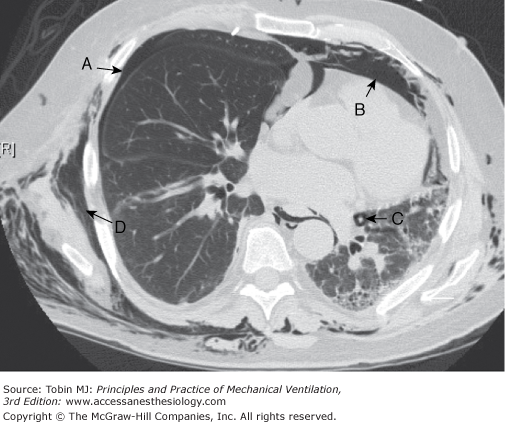
An example in the ICU may be morbid obesity where the weight placed upon the chest wall results in an increase in both pleural pressure and plateau pressure.Ī more physiologically-exciting example is that of fighter-pilots wearing anti-gravity suits. When considering the stress or pressure across the lung one can anticipate clinical scenarios whereby both plateau and pleural pressure rise in tandem such that the plateau pressure is very high, but because the pleural pressure is also high, the pressure across the lung is actually normal. Analogous to volume, it is not solely the value of pressure in the airway that is important, but rather the pressure in the airway relative to the pressure around the lung – the pleural pressure. Pressure is often measured clinically as the plateau pressure on the ventilator. The pressure across a distensible material is known as stress and is directly related to strain - see equation 1.Įquation 1 : stress and strain are directly related by a constant - K - the specific elastance If the volume of the baby lung is unknown, true lung strain is also unknown but it is clear that keeping tidal volume small will also keep lung strain small. However, in the second patient, the same tidal volume results in a lung strain of 5.0 ! These two extreme examples illustrate why there is no one-size-fits-all tidal volume for all patients with ARDS. Lung strain is the tidal volume divided by the FRC. Delivery of 500 mL to the first patient results in a lung strain of 0.33. Imagine, for example, two different patients – one with an FRC of 1500 mL and the other with an FRC of only 100 mL because of severe lung injury. The latter is often referred to as the ‘baby lung’ in ARDS because FRC can be quite variable and quite small FRC in ARDS is typically unknown. However, equally-important is the absolute volume delivered relative to the baseline volume of the lung. The absolute volume applied to the lung is an important determinant of biological injury. I hope to clarify these two processes by sewing together basic physiological principles and clinically-relevant values into a pleasing patchwork quilt of ICU physiology. Last spring – in Montreal – I was asked a few questions about volutrauma and its relationship to barotrauma. Pulmonary barotrauma may be more likely in those with damage from previous or current lung conditions.In a recent and excellent open-access review, Gattinoni, Quintel and Marini ask which is worse, volutrauma or atelectrauma ? This concise review is an absolute must-read and forms the fabric from which this short article assembles. Structural defects of the sinuses or their drainage system.Similarly, blockages in the sinuses will block the flow of air from outside to inside the body. Damaged or blockage of eustachian tube-resulting from scarring or a tumor.Defects of eustachian tube (small tube that runs from the middle ear to the back of the nose and upper throat and helps stabilize internal and external pressures).Middle ear infections-more common in younger children.These tubes may be blocked or limited by: Blockages and congestion in these tubes increase the risk of ear barotrauma because the inside pressure is not allowed to change to match the outside pressure. The inner ear is connected to outside air through tubes to keep inner and outer pressure balanced. Exposure to shock waves from an explosion.use of a machine to move air into and out of the lungs (associated with pulmonary trauma) Having air pockets in equipment (such as masks and dry suits).Underwater diving for an increased period of time.Swimming quickly to the surface when diving.Ascending (going up to the surface) without exhaling freely.Activities that can expose someone to significant pressure changes include:
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
